Almost before the dust had settled on the agreement that sealed the coalition between the Conservatives and the Liberal Democrats after the May 2010 election, Tory health secretary Andrew Lansley announced plans that shook the partnership to the core - to overhaul the National Health Service.
A flurry of drafts, “listening exercises” and almost 16,000 consultation responses followed. But while politicians, doctors, journalists and lobby groups debated privatisation and the question of who should hold the purse strings, another quieter group put forward its demands.
Organisations - including medical academies, universities, industry and charities - were determined to cement a focus on research within the NHS that had been growing since 2006.
They called for the widespread changes that had previously turned parts of the service upside down to be consolidated, and for guarantees that the general practitioners in control of the new system would not neglect their research responsibilities.
The Health and Social Care Act 2012 became law in March, and has met many of these demands. But as the reforms begin to be implemented, patients and clinicians are still in the dark about many aspects of the system that goes live in April 2013.
The main change will be to replace primary care trusts and strategic health authorities with 210 clinical commissioning groups (CCGs); local consortia, led by GPs, which will allocate resources for everything from hospital care to community services, and which will act as their patients’ gateway to clinical research.
A familiar face, for academics at least, will be at the helm during the transition. Malcolm Grant, currently the provost of University College London, will chair the NHS Commissioning Board, which at national level will bring together the commissioning groups and their £80 billion budget.
Originally a barrister and environmental lawyer, Grant has experience both with the workings of government and the life sciences, having overseen UCL’s role in founding the £700 million Francis Crick Institute, a collaboration with the government and medical research charities.
With controversy surrounding the NHS reforms, Grant’s decision to take on the role - announced in 2011 as a part-time one, although he has since said he will step down from UCL’s leadership at the end of the 2012-13 academic year - was criticised by UCL students, leading to a failed vote of no confidence in his leadership. But Grant says he supports the government’s goal of creating a system that is more “local” and “needs-led” while also being more competitive and efficient.
He told Times Higher Education that although reforming the NHS would be a “very long, complex and difficult process”, he firmly believed that through it, research would be reinforced and standards would improve.
“First of all there’s a statutory duty in the new legislation, on the secretary of state, on us and all the other bodies including clinical commissioning groups not only to commission research but to use the results of research in operations.
“It’s the first time there has been such a duty and I think those duties are potentially very powerful,” he says.
CCGs could choose to specify in contracts that healthcare providers should promote recruitment of patients for research, for example, or systematically collect data for national research repositories - but such decisions will be up to each group.
So far, however, not one of the 40 most advanced groups explicitly mentions research in its plans.
Some hospital clinicians worry that crucial research, especially into rare diseases, could slip through the cracks in the fragmented system, led by a group of clinicians who are not traditionally engaged with research.
Organisations such as the Association of Medical Research Charities have told the government of their concern that CCGs may be reluctant to pay the additional patient care costs associated with research.
Grant says the CCGs are a work in progress and insists that the NHS Commissioning Board will not allow research to be forgotten.
“I’m fully conscious of the risks of fragmentation with CCGs and we, the board, are going to be working very closely with them in the collective as well as individually. I suspect that much of the research drive will be in the collective.
“We have to be scrupulous to ensure that there is no loss of focus on quality, safety and improvement of healthcare while the new system is brought into effect.”
In fact, Grant sees the loosening of political control over local commissioning as a chance to change what he sees as the NHS’ traditional reluctance to innovate, allowing it to make better use of research results.
“In the private sector, if someone comes up with a new wi-firouter, the first thing every other company does is take it apart, look at how it works and try to figure it out for themselves.
“Instead, the NHS’ approach has always been the opposite; to (dismiss it with) ‘it wasn’t invented here’.
“CCGs will have responsibility for outcomes but great space for initiative and innovation,” Grant argues.
Dame Sally Davies, director general of research, chief scientific adviser and chief medical officer at the Department of Health, says her department has an agreement with the board that before gaining full authorisation, the CCGs will have to show they are “research ready”.
“It’s going to take time; it’s a changed management process. But this government, like the previous government, wants this to happen,” Davies says.
Researchers’ fears for the future role of research within the NHS stem in part from concerns that the progress that has been made since 2006 could be undermined.
Six years ago, when the venture capitalist Sir David Cooksey embarked on an independent review of how best to fund health research in the UK, the situation was far from rosy.
Despite continued strengths in the UK’s basic sciences, Sir David found that clinical development was falling to pieces.
Through the 1980s and 1990s the number of NHS staff involved in research fell by around two-thirds, he observed. The number of clinical trials also fell, with the Academy of Medical Sciences recording that the UK’s share of global patient recruitment dropped from 6 per cent in 2000 to between 2 and 3 per cent in 2006.
Meanwhile, modest NHS funding for research was spread out across a system that many felt was resistant to innovation and in which relationships with industry and the academy were patchy.
“There was research going on but it was not properly supported, timelines and delivery were hindered and there were no real quality measures,” attests Christine McGrath, director of research and development at University Hospital Southampton.
Cooksey’s report, A Review of UK Health Research Funding, published in December 2006, fanned the flames started by Davies in the strategy Best Research for Best Health published in January that year.
Recognising the lack of focus in provision, Davies first withdrew the research funding that was embedded across NHS trusts and then pulled it into a single National Institute for Health Research that could both overlay the regular health service and draw in researchers from the academy.
She also persuaded the Labour government of the day to boost and ring-fence the department’s annual research and development budget to £1 billion by 2010-11.
“The government’s agenda (from) 2006 changed the landscape in such a phenomenal way,” says McGrath. “Across the NHS, apart from the Golden Triangle (Oxford, Cambridge and some London universities) perhaps, research really was a low priority, but the NIHR has really put it up the agenda.”
At the centre of the changes was the creation of NIHR biomedical research centres, hospital and university collaborations intended to translate lab-based discoveries into cutting-edge treatments and to encourage the health service to take up innovations (see box, below).
The 12 centres - five comprehensive and seven specialist - were formed around geographical and existing collaborations, in areas that had universities with particular academic strengths in medical research, and chosen in open competition.
Work started slowly, with the centres sharing a modest £50 million in 2007, before funding doubled the following year and increased until 2011-12.
But Patrick Chinnery, director of Newcastle’s NIHR Biomedical Research Centre in Ageing, which involves Newcastle upon Tyne Hospitals NHS Foundation Trust and Newcastle University, says the investment was a game-changer. “It forced a culture change that made those organisations work much closer together, to jointly get their act together and push in the same direction,” he says.
Tension between academic and hospital goals often meant that the two groups pulled in different directions. The research assessment exercise, for example, encouraged academics to focus on easy-to-measure research papers rather than lengthy and expensive clinical trials, while hospitals concentrated on short-term delivery and balancing the books.
But tying the core business of each together through the centre made research and its translation a priority at the level of university deans and healthcare trust chief executives, Chinnery says, adding that it “allows the trust chief executive to have the space to keep research on his agenda as core business while university researchers get funding and recognition for clinical research”.
Aligning training within the centres has also encouraged the development of PhD students, nurse and allied healthcare professionals who bridge the divide, Chinnery continues.
“The whole problem is that for many years there has been parallel working in hospitals and universities, speaking different languages. We’re trying to train individuals in speaking both languages, to get research converted into biomarkers and treatments.”
The system seems to be working. The UCL Institute of Ophthalmology and Oxford’s Biomedical Research Centre, for example, can cite success in bringing cutting-edge gene therapy, developed through research at Imperial College London, through to clinical trials for the rare degenerative blindness choroideremia.
Sir John Tooke, vice-provost for health at University College London and president of the Academy of Medical Sciences, says that by working with universities, the NHS not only strengthens education and accelerates research but improves care.
“I think there’s a recognition among the more enlightened hospitals … that research-engaged hospitals are more likely to adopt evidence-based practice, and therefore the overall standard of care is lifted.”
And there is evidence that university hospitals outperform others. According to the vice-chancellors’ body Universities UK, university hospitals are more likely to have below-average mortality rates than other hospitals.
“I think it’s having a critical culture, being a challenging, learning organisation and the association of academia with the health service that enables that,” Tooke adds.
Funding for research did not stop at the 12 centres. In a bid to fill gaps in priority areas left out by larger centres, the government created biomedical research units.
Launched in 2008 at a wider range of institutions - including the University of Birmingham and Queen Mary, University of London - these 15 mini-partnerships each received around £1 million a year.
To bring the research together, the government also established five academic health science centres, with the first of them, Imperial College Healthcare, launched in 2007. These were designed not to fund research directly but to keep different NIHR-funded centres abreast of each other’s work, identify key academic and clinical themes and spread the evidence they generated into practice more widely.
According to UCL’s Grant, these academic health science centres have worked as much to improve relationships within the NHS as between the NHS and higher education institutions. “It’s almost as if, at least at one level, universities have given a neutral territory for conversations within the NHS about improving quality and safety of care,” he says.
Grant attributes the “spectacular” 40 per cent improvement in 90-day survival rates across acute stroke units in London to the greater specialisation and use of the evidence base enabled by one of London’s academic health science centres, University College London Partners.
“You’re starting to see the whole area of London becoming more aligned in healthcare and with universities playing a central role,” he says. “But it’s not perfect and there’s a long way to go.”
Four years in, the promise of the system helped Davies to secure a commitment in the 2010 Comprehensive Spending Review that health research funding would increase in real terms until 2015, the only area other than international development to receive an increase.
This April, funding increased for all three systems - NIHR biomedical research centres and biomedical research units, and academic health science centres - in a second round of allocation (see graphic, page 35). Between 2012 and 2017, 11 biomedical research centres will share £775 million in funding, while 20 biomedical research units will divide £126 million among themselves.
Davies believes that the centres have been transformational. “The whole thing is beginning to buzz. If you go back to 2005, universities and hospitals were in different places, but they (now) realise if they don’t work through the partnership both will suffer, not just in research funding: (they won’t) be attractive for the students and they won’t be delivering the best service for their patients.”
Last year, 97 per cent of hospital trusts were carrying out at least one clinical study. “We’re increasing the number of patients recruited to trials year on year. Last year 565,000 patients were put into studies, and we’re doing more with industry, with more than 1,000 studies open,” Davies says.
Spreading the innovation that has been pioneered in elite academic centres across the service will be the next priority. Last month the NHS opened applications to set up academic health science networks, between 12 and 18 organisations that it hopes will link major universities to every local NHS organisation and local care service.
“One of the things we’ve … learned from academic health research centres is that you can get a significant common purpose towards research and innovation, which includes organisations that would otherwise have been excluded and (that traditionally) see research as something otherwise done in ivory towers,” says Sir Bruce Keogh, national medical director on the new NHS Commissioning Board.
The flip side to the range and scale of efforts under way to boost research in the NHS is the pressure to deliver, says Newcastle’s Chinnery.
“There’s enormous pressure on us to deliver the NIHR dream. If, when the next spending review comes, we’re not delivering what the NIHR said it would deliver (namely, translating research into improvements in care), this funding is absolutely under threat and correctly so.”
A lack of patient engagement in clinical trials remains one of the greatest hurdles to overcome. Although the NIHR’s Clinical Research Network recruited more than half a million people into research studies last year, awareness among patients remains low.
A survey conducted on behalf of the network in May found that only 21 per cent of the public were aware that carrying out research is a key activity for the NHS.
Another long-standing thorn in the side of researchers and the pharmaceutical industry alike are the regulatory hurdles to clinical trials. While it takes an average of 70 days to recruit the first patient to a clinical trial in Scotland, the same task in England, where approval must be sought from each trust in which patients are recruited, takes 363 days.
Sharmila Nebhrajani, chief executive of the Association of Medical Research Charities, says the issue is frustrating because studies routinely show that the public are willing participants.
“Although the NHS is called a national health service it isn’t really national at all. It’s a complex web of local organisations knitted together.
“That can be a good thing, as it means it’s focused on serving the local population, but it means bureaucracy makes life difficult,” she says.
Davies says that yet another work in progress, the newly established Health Research Authority, will streamline authorisation with a single application system and a more proportionate approach to risk.
She hopes this will help trusts to meet ambitious NIHR targets to reduce the time to recruit first patients to an average of 70 days.
But the new authority won’t reduce the number of approvals, and each trust will still need to obtain the go-ahead individually. “The big issue is locally how trusts handle governance permissions,” Davies explains. “The HRA can help oil the wheels but it’s the legal duty of the trust to decide whether they will host research or not.”
As the reforms unfold, the final challenge will be to improve the way the NHS harnesses data and uses them for research and improving care, Keogh says.
In the past, efforts to make use of the NHS’ status as the largest integrated healthcare system in the world have been stymied by the failures to synchronise technology between GPs and trusts, the low priority given to data collection and patient fears over privacy.
“The NHS misses out on the opportunity to roll out the fruits of research as quickly as it could,” Keogh says.
One remedy could be the Clinical Practice Research Datalink. Opened in late March, the service acts as a gateway for researchers and patients to existing anonymised data and gives advice on recruitment and methodology.
Grant says he hopes the NHS Commissioning Board will also provide a framework within which to standardise and link up data, while better information on how data are used can convince patients to take part.
“Over the whole of the UK we have something like 65 million people, nowhere else in the world has got that (in a single healthcare system),” he says, before adding: “But we’ve got a long way to go.”
SILVER FOR GOLD: EQUALITY MEASURES
Medical research is the only field in which budgets have continued to rise rather than fall during the UK’s financial crisis, so the Department of Health has not hesitated to attach some strings to the funding.
Last year Sally Davies, the department’s chief scientific adviser and chief medical officer, quietly announced that to be shortlisted for the next round of biomedical research centres in 2016, institutions must meet gender equality criteria.
In order to get a cut of the £800 million programme, universities will have to hold an Athena SWAN award, organised by the Equality Challenge Unit, of at least silver level. Currently, just 15 health or bioscience departments in UK universities have achieved this status, with only one UK institution holding a gold award.
The awards go to departments that can show progress in hiring and retaining women, providing career support, helping to achieve a better work-life balance, and demonstrating gender equality in making senior appointments.
“It’s been welcomed by women not just in academic medicine but in the NHS and other science subjects,” says Davies.
“And the universities have generally recognised there’s a need to be seen to do something (in this area).”
The Equality Challenge Unit is expecting interest to soar and the Department of Health has given the organisation £200,000 to build its capacity in anticipation.
Davies’ move has inspired other funders, and the research councils are now said to be in talks with the unit about ways to tie funding to equality commitments.
TIMELINE: RECENT MILESTONES IN UK HEALTH RESEARCH AND DEVELOPMENT
2004: The government focuses on “health and wealth” in its 10-year Science and Innovation Investment Framework (up to 2014).
2006: The National Institute for Health Research is established in England as a framework for a “complete health research system”.
2007: The first batch of biomedical research centres and academic health science centres are established.
2008: Biomedical research units added.
2009: Publication of the new NHS Constitution, which includes a “commitment to the promotion and conduct of research to improve the current and future health and care of the population”.
2010: The Comprehensive Spending Review commits the government to increasing spending on health research in real terms, with an additional focus on research translation.
March 2011: The government’s Plan for Growth sets a 70-day maximum start-up time for NIHR-funded trials and plans for a Health Research Authority to decrease red tape. It also sets a commitment to increase public information on clinical trials and build consensus using e-health record data.
December 2011: Publication of the NHS chief executive’s report Innovation, Health and Wealth, which includes a commitment to establish academic health science networks.
March 2012: Passage of the Health and Social Care Act 2012. It includes a duty for the secretary of state for health, the NHS Commissioning Board and clinical commissioning groups to promote research, promote the use of its evidence and support its conduct.
JOINED-UP SOLUTIONS: SOUTHAMPTON’S BIOMEDICAL RESEARCH UNITS
The Nutrition, Diet and Lifestyle Biomedical Research Unit and the Respiratory Biomedical Research Unit are collaborations between the University of Southampton and University Hospital Southampton NHS Foundation Trust.
Although it is far from the largest trust, Southampton puts the second-highest number of patients through clinical trials of any in the country, and the figure is rapidly rising, up from about 7,000 in 2009-10 to 14,826 in 2011-12.
Just six years ago the number of trials under way could be counted on one hand, but now the figure is in the hundreds and the trust sits in the country’s top five in terms of commercial collaboration.
“Buy-in from both sides” was crucial to making the partnership work, says Alan Jackson, professor of human nutrition and director of the Nutrition, Diet and Lifestyle BRU.
The studies are led either by NHS consultants who fit research around their normal activity or by clinical academics employed by the university who see patients in addition to performing their academic role.
Clinical support, such as nurses, radiographers and pharmacists, bring the total number of staff under the BRU umbrella to around 100.
The NIHR centre, built on an existing university-hospital collaboration, the Institute of Human Nutrition, created a structure to easily import information gained from research into training and practice, says Jackson.
“It couldn’t have happened otherwise. It’s very difficult to achieve that unless you have the clinical work and research work taking part in the same place because it’s such a complicated area,” says Jackson.
Both centres have already proved their worth, with research being instrumental in creating NHS guidelines on managing patients with nutritional problems, proving that giving vitamin D supplements to pregnant women could enhance children’s bone development and doing the largest share of the studies that underpinned the government’s swine flu vaccination strategy.
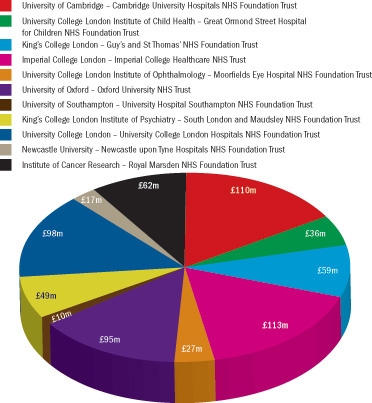
Biomedical Research Centre Allocations 2012-2017
The Comprehensive Spending Review of 2012 allocated 11 biomedical research centres a share of £775 million between 2012 and 2017
Register to continue
Why register?
- Registration is free and only takes a moment
- Once registered, you can read 3 articles a month
- Sign up for our newsletter
Subscribe
Or subscribe for unlimited access to:
- Unlimited access to news, views, insights & reviews
- Digital editions
- Digital access to THE’s university and college rankings analysis
Already registered or a current subscriber?




